Small White Spots on Your Skin? Here’s What Your Body is Trying to Tell You
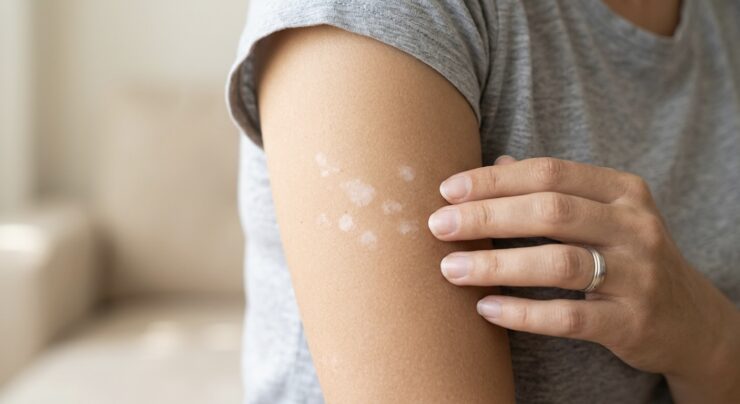
Human skin has a remarkable way of communicating with us. It flushes red when we feel embarrassed, breaks out in goosebumps when we’re cold, and sometimes develops tiny white patches that seem to appear without warning.
If you’ve recently noticed small white spots or pale patches on your skin, there’s no need to panic. You’re definitely not the only one. For many people, the first reaction is fear. Thoughts immediately jump to fungal infections, permanent skin damage, or hidden health issues happening inside the body.
Thankfully, most white spots that appear on the skin are medically harmless. Still, because our skin plays such a major role in self-confidence and appearance, it’s natural to want answers. In most cases, these pale areas develop because melanin — the pigment responsible for giving skin its color — either decreases or stops being produced in certain spots altogether.
Below, we’ll break down the most common reasons these white patches appear, how each condition develops, and what can actually be done about them.

1. The Most Likely Culprit: Idiopathic Guttate Hypomelanosis (IGH)
If you’re over 30 and have started noticing tiny porcelain-white spots on your forearms or shins, there’s a good chance you’re dealing with Idiopathic Guttate Hypomelanosis, commonly shortened to IGH. Although the medical name sounds intimidating, it’s actually one of the most common harmless skin conditions.
The term itself explains the condition: “idiopathic” means the cause is unclear, “guttate” refers to the tear-drop shape, and “hypomelanosis” means reduced pigmentation. Research published in dermatology journals suggests that IGH is largely linked to aging skin combined with years of sun exposure. Over time, ultraviolet rays gradually damage melanocytes — the cells responsible for producing pigment — until some simply stop functioning in isolated areas.
Appearance: Small flat pale spots with a smooth surface, usually measuring between 2mm and 5mm.
Location: Most commonly found on the shins and forearms, though they may occasionally appear on the face or upper back.
According to the American Academy of Dermatology, IGH is purely cosmetic and is not connected to skin cancer.
What can be done
Because the pigment-producing cells in these spots often stop working completely, restoring color can be difficult. The best prevention is limiting additional UV exposure so more spots don’t form over time. Some dermatologists may recommend topical retinoids or mild dermabrasion treatments to soften their appearance, but many people simply choose to leave them alone.

2. The Living Landscape: Tinea Versicolor
Not all white spots are caused by sun damage. In some cases, they’re linked to something naturally living on your skin: yeast.
Tinea versicolor is a fungal condition caused by an overgrowth of yeast called Malassezia. This yeast naturally exists on everyone’s skin as part of the normal microbiome. However, hot weather, humidity, excessive sweating, or oily skin can allow it to multiply too quickly. Once that happens, the yeast produces substances that interfere with melanin production, leading to lighter — and sometimes darker — patches on the skin.
Appearance: White, pink, or light-brown patches with a thin, slightly scaly surface that becomes more noticeable when gently scratched.
Behavior: The spots usually stand out more after sun exposure because the surrounding skin tans while the affected areas do not.
The Centers for Disease Control and Prevention notes that this is among the most common superficial fungal skin infections worldwide.
How to manage it
Tinea versicolor is usually treated with over-the-counter antifungal creams such as clotrimazole or miconazole. Dermatologists also frequently recommend anti-dandruff shampoos containing selenium sulfide or ketoconazole, used as a body wash. Typically, the product is applied to the affected area, left on for five to ten minutes, and then rinsed away.

3. Pityriasis Alba: The Dry Skin Connection
Pityriasis alba is often mistaken for more serious skin conditions, especially in children and teenagers. It’s commonly associated with dry skin and is considered a mild form of eczema, also known as atopic dermatitis.
Unlike IGH, which produces smooth white spots immediately, pityriasis alba usually begins as slightly red, irritated, and flaky patches. Once the inflammation settles down, pale dry areas remain behind. It’s especially common in children who also deal with asthma, allergies, or hay fever.
Appearance: Round or oval pale patches usually found on the cheeks, chin, or upper arms.
Seasonality: The condition becomes more noticeable during summer because the surrounding skin tans while the pale patches stay lighter, creating stronger contrast.
DermNet NZ describes pityriasis alba as a self-limiting condition, meaning it often fades naturally over time as children grow older.
Treatment and Care
Hydration is the main focus here. Thick fragrance-free moisturizers applied twice daily can help restore the skin barrier and reduce dryness. If the patches become red or irritated, a mild over-the-counter hydrocortisone cream may help calm the inflammation for a short period.

4. Vitiligo: When the Immune System Intervenes
One of the most recognized causes of white patches is vitiligo, an autoimmune condition in which the immune system mistakenly attacks the body’s own melanocytes.
Vitiligo differs from other conditions because the pigment loss is usually complete. Instead of pale areas, the skin becomes sharply “milky white.” The condition affects around 1% of people worldwide and can begin at almost any age.
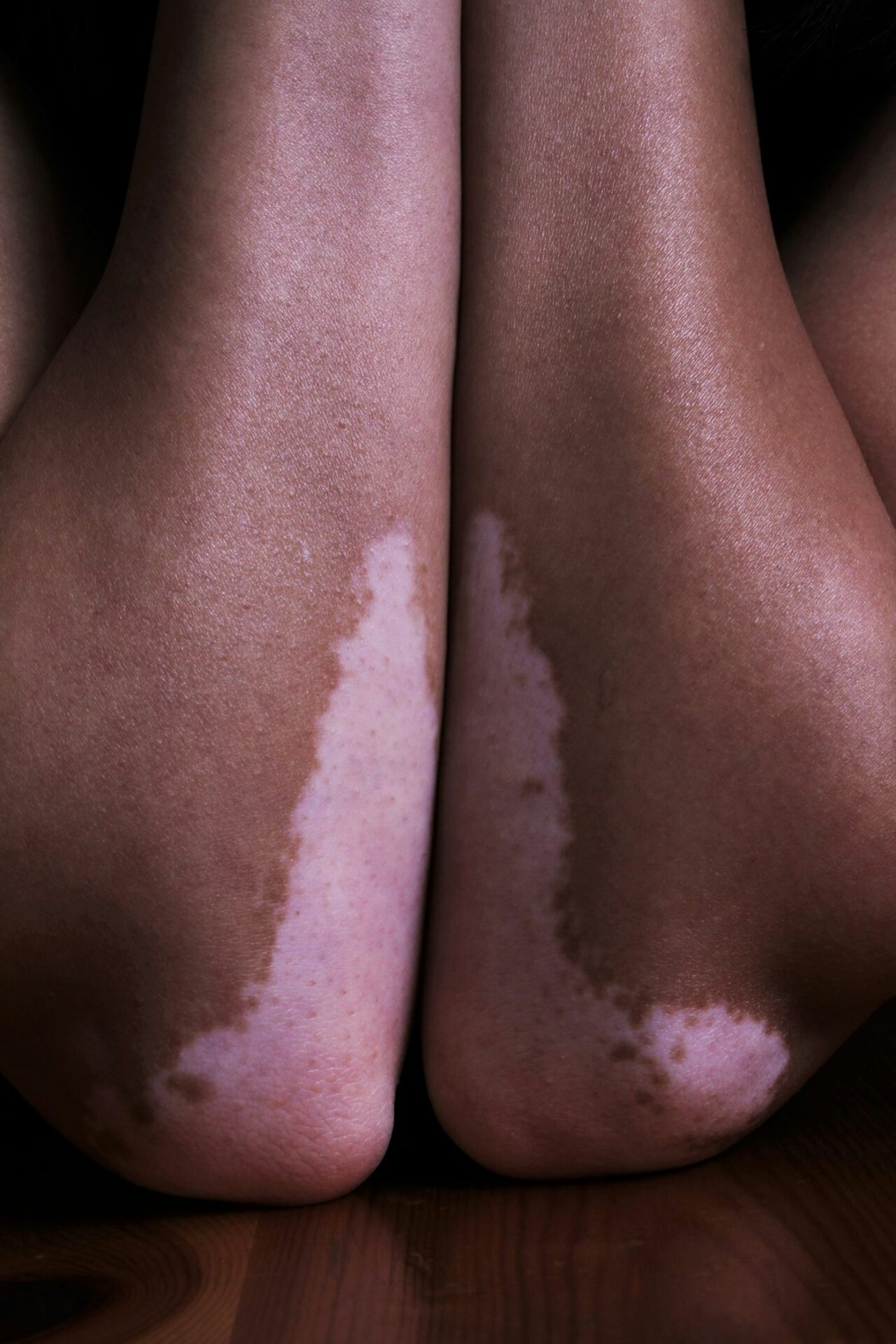
Appearance: Bright chalk-white patches with clearly defined borders, often appearing symmetrically on areas like both elbows, both knees, or both sides of the face.
Course: Some individuals develop only a few stable patches, while others may experience gradual spreading over many years.
The National Institute of Arthritis and Musculoskeletal and Skin Diseases emphasizes that although vitiligo is not painful or contagious, it can carry significant emotional and psychological effects.

Modern Medical Breakthroughs
Treatment options for vitiligo have improved dramatically in recent years. Therapies now include UVB light treatment, topical steroid creams, and newer medications known as JAK inhibitors, which help calm the immune response and may allow pigment to return in some areas. If you suspect vitiligo, consulting a dermatologist is strongly recommended.
Distinguishing the Difference: A Quick Reference
If you’re trying to identify which condition most closely resembles your skin changes, here’s a simple comparison:
| Feature | IGH (Sun Spots) | Tinea Versicolor | Pityriasis Alba | Vitiligo |
| Texture | Smooth | Slightly Scaly | Dry/Rough | Smooth |
| Edges | Blurry/Small | Defined | Faded/Blurry | Very Sharp |
| Itchiness | Never | Sometimes | Rarely | Never |
| Typical Age | 30+ | Teens/Young Adults | Children | Any |
| Sun Impact | Caused by sun | More visible after sun | More visible after sun | Higher burn risk |
Essential Skin Care Strategies
No matter what’s causing the white patches, skin protection and barrier support remain extremely important.
The Non-Negotiable: SPF 30+
When skin loses pigment, it also loses part of its natural defense against UV damage. White patches burn more easily than surrounding skin, which is why daily sunscreen use matters so much — even on cloudy days. Dermatologists often refer to the resulting visible difference as the “contrast effect.”
Barrier Repair
For conditions like pityriasis alba or chronic dry skin, restoring moisture is essential. Many dermatologists recommend the “moisture sandwich” method: apply water or a hydrating serum first, then immediately seal it in with a thick ceramide-rich moisturizer.
Balance Your Microbiome
If fungal flare-ups like tinea versicolor keep returning, breathable clothing can help. Cotton and linen fabrics allow airflow and reduce trapped sweat, while synthetic materials such as polyester tend to hold heat and moisture against the skin, creating an ideal environment for yeast overgrowth.
When to See a Professional
Although the conditions listed above are among the most common explanations for white spots, there are rarer disorders — including Lichen Sclerosus and certain forms of skin lymphoma — that may also cause pale patches.
You should consider seeing a dermatologist if:
- The spots appear suddenly and spread quickly.
- The skin becomes thickened, painful, or starts bleeding.
- The patches develop around the genital area.
- The pigment loss is causing severe emotional distress.
Dermatologists may use a Wood’s Lamp, a specialized ultraviolet light used in dark rooms to examine the skin more closely. Under this light, vitiligo often glows a bright blue-white color, while fungal infections may appear yellow or green, helping doctors make a faster and more accurate diagnosis.